Bladder Removal Surgery (Cystectomy)
Surgical Care Explained
Cystectomy (Bladder Removal Surgery): What You Need to Know
Cystectomy (sis-TEK-tuh-me) is a surgical procedure to remove the urinary bladder. It is most commonly recommended for people with invasive or recurrent bladder cancer, but it may also be advised for certain advanced pelvic cancers or specific non-cancerous conditions.
In men, a radical cystectomy usually involves removal of the bladder along with the prostate and seminal vesicles.
In women, the procedure may include removal of the bladder, uterus, ovaries, and a small portion of the vagina.
After the bladder is removed, your surgeon will create a urinary diversion—a new pathway that allows urine to be stored and pass out of your body. There are several safe and effective options available. Your doctor will carefully explain these choices and help you select the one that best suits your lifestyle, health needs, and recovery goals.
Cystectomy may be recommended to treat:
Invasive or recurrent non-invasive bladder cancer
Advanced pelvic cancers (such as colon, prostate, or endometrial cancer)
Severe non-cancerous conditions, including interstitial cystitis
Certain congenital (birth-related) urinary abnormalities
Patient Education & Surgical Care
Cystectomy (Bladder Removal Surgery): Reasons, Procedure, Risks & Recovery
When other treatments are not effective, cystectomy can be a life-saving procedure that offers the best chance for long-term control, symptom relief, and improved quality of life.
Your doctor may recommend a cystectomy (surgical removal of the bladder) to treat:
- Bladder cancer or cancers nearby that have spread to the bladder
- Congenital (birth) defects affecting the urinary system
- Neurological or inflammatory conditions that damage bladder function
The type of cystectomy and urinary reconstruction depends on the reason for surgery, your overall health, and your personal preferences. Your surgeon will help you choose the safest and most suitable option.
Cystectomy is a major abdominal surgery and carries certain risks, including:
- Bleeding and infection
- Blood clots
- Heart or lung complications (such as pneumonia)
- Rarely, life-threatening complications
Because cystectomy also involves creating a new way for urine to leave the body (urinary diversion), additional risks may include:
- Dehydration or electrolyte imbalance
- Urinary tract infections
- Bowel obstruction
- Blockage of the ureters (tubes carrying urine from the kidneys)
Some complications may require additional surgery or hospital readmission. Your surgeon will explain risks specific to your case.
Before surgery:
- Inform your doctor about all medications, supplements, alcohol, caffeine, or drug use
- You may need to stop or adjust certain medicines
- Quit smoking if you smoke—this greatly reduces surgical risks and improves healing
You will receive clear pre-surgery instructions. Always ask questions if anything is unclear.
During surgery, your surgeon removes the bladder and nearby lymph nodes.
- In men: the prostate and seminal vesicles are usually removed
- In women: the uterus, ovaries, and part of the vagina may be removed
A new pathway for urine is created during the same operation.
Surgical Approaches
Your surgeon may use:
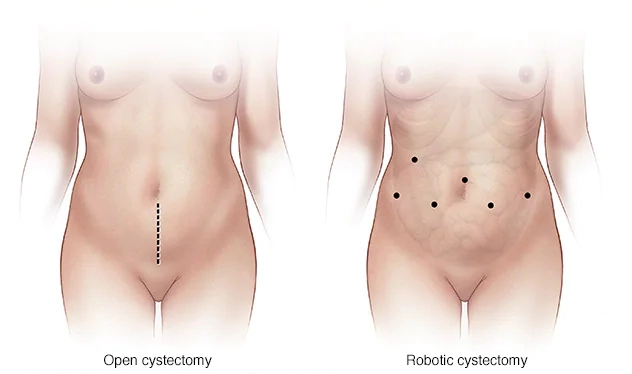
- Open surgery: one larger abdominal incision
- Minimally invasive surgery: several small incisions
- Robotic surgery: a minimally invasive approach using robotic assistance
All procedures are done under general anesthesia.
After bladder removal, one of the following may be created:
-
Ileal Conduit
- A small piece of intestine forms a tube that drains urine to an opening (stoma) on the abdomen
- Urine collects in a pouch worn outside the body
- Neobladder Reconstruction
- A new bladder is created using intestine and connected to the urethra
- Allows near-normal urination
- May require temporary catheter use and bladder training
- Continent Urinary Reservoir
- An internal pouch stores urine
- You drain it using a catheter several times a day
- No external urine bag is needed
- Hospital stay: 5–6 days on average
- Walking soon after surgery helps prevent complications and speeds recovery
- Pain and discomfort are common initially but improve over time
Urinary Changes
- Some blood or mucus in urine is normal early on
- Mucus occurs because intestine tissue is used—this decreases over time
Regular follow-ups help ensure:
- Proper kidney drainage
- Stable electrolyte levels
- Early detection of cancer recurrence (if surgery was for cancer)
- Limit lifting, driving, and strenuous activity for 6–8 weeks
- Gradually return to work and normal routines
- Sexual activity can usually resume after about 6 weeks, with your doctor’s approval
Cystectomy can significantly improve health and quality of life. Most people return to normal daily activities with time and support.
- With a stoma: confidence grows as you learn care techniques
- With a neobladder: bladder capacity increases gradually over months routines
Sexual changes can occur:
- Men: temporary or permanent erectile difficulties may happen; treatments are available
- Women: vaginal changes may affect comfort; nerve-sparing options may help
Intimacy is still possible—even with a stoma. Open communication with your partner and care team is key.
If you’re considering or have been advised to undergo cystectomy, schedule a consultation with an experienced surgeon. Understanding your options empowers you to make confident, informed decisions about your health.
