Abdominal Hysterectomy
Understanding Your Surgical Care
Abdominal Hysterectomy: What It Is and When It’s Recommended
An abdominal hysterectomy is a surgical procedure in which the uterus (womb) is removed through a small incision in the lower abdomen. The uterus is the organ where a baby develops during pregnancy.
There are different types of hysterectomy, depending on what needs to be removed:
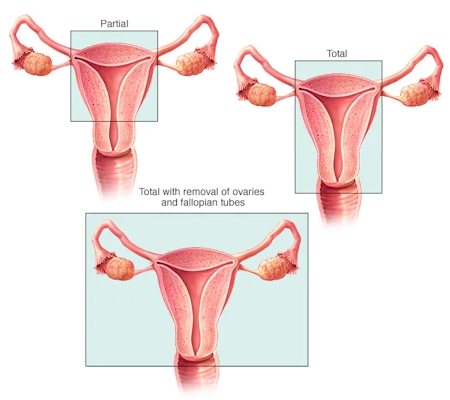
Partial (subtotal) hysterectomy: Only the uterus is removed; the cervix is left in place.
Total hysterectomy: Both the uterus and cervix are removed.
Total hysterectomy with salpingo-oophorectomy: The uterus, cervix, and one or both ovaries and fallopian tubes are removed.
A hysterectomy can be performed in several ways, including through the vagina, or using minimally invasive laparoscopic or robotic techniques. However, in some cases, an abdominal approach is the safest and most effective option.
Your doctor may recommend an abdominal hysterectomy if:
The uterus is significantly enlarged
There is a need to closely examine other pelvic organs
Your surgeon believes this approach offers the best outcome for your condition
If you’ve been advised to undergo an abdominal hysterectomy, a personalized consultation can help you understand your options, recovery, and expected results—so you can move forward with confidence and clarity.
Women’s Health & Surgical Care
Hysterectomy: Why It’s Done, What to Expect, and Life After Surgery
A hysterectomy is a surgical procedure to remove the uterus. It is recommended when other treatments are ineffective or when the condition is serious. Your gynaecologist will advise this option only after careful evaluation of your symptoms, diagnosis, and future reproductive plans.
You may need a hysterectomy to treat:
-
Gynaecologic cancers
Conditions such as cancer of the uterus, cervix, or ovaries may require a hysterectomy as the most effective treatment. Depending on the stage and type of cancer, surgery may be combined with radiation or chemotherapy. -
Uterine fibroids
Fibroids are non-cancerous growths that can cause heavy bleeding, anemia, pelvic pain, or pressure on the bladder. A hysterectomy is the only permanent solution when symptoms are severe and other treatments fail. -
Endometriosis
When uterine lining tissue grows outside the uterus and does not respond to medication or conservative surgery, hysterectomy—sometimes along with removal of ovaries and fallopian tubes—may be advised. -
Uterine prolapse
Weakening of pelvic support structures can cause the uterus to descend into the vagina, leading to urinary problems, pelvic pressure, or bowel issues. Hysterectomy can effectively relieve these symptoms. -
Abnormal or heavy menstrual bleeding
If bleeding is excessive, irregular, or prolonged and cannot be controlled with medication or minimally invasive procedures, hysterectomy may provide long-term relief. -
Chronic pelvic pain (uterine origin)
In select cases where pain is clearly linked to the uterus and all other treatments have failed, hysterectomy may be considered as a last option.
Important: A hysterectomy ends the ability to become pregnant. If you may wish to conceive in the future, discuss fertility-preserving alternatives with your doctor. For cancer, surgery may be essential, but for other conditions, less invasive options are often available.
In some cases, your surgeon may also recommend removing both ovaries and fallopian tubes (bilateral salpingo-oophorectomy). This can lead to surgical menopause, where menopause symptoms begin suddenly. Hormone therapy may be suggested to manage symptoms and maintain quality of life.
Hysterectomy is generally safe, but as with any major surgery, there are potential risks, including:
- Infection
- Blood clots
- Excessive bleeding
- Reaction to anesthesia
- Injury to nearby organs (bladder, urinary tract, bowel)
- Earlier onset of menopause (even if ovaries are preserved)
- Rarely, serious complications
To feel confident and prepared:
- Get informed: Ask questions and understand the procedure and recovery process.
- Review medications: Inform your doctor about all medicines, supplements, or herbal products you take.
- Discuss anesthesia: Abdominal hysterectomy is usually done under general anesthesia.
- Plan recovery: Hospital stay is typically 1–2 days; full recovery may take several weeks.
- Arrange support: You may need help at home during the initial recovery period.
During an abdominal hysterectomy, the uterus is carefully separated from surrounding tissues and removed. Depending on your condition, the cervix, ovaries, and fallopian tubes may also be removed. The procedure usually takes 1–2 hours and is performed under general anesthesia.
- Hospital stay: 1–2 days (sometimes longer)
- Mild to moderate pain managed with medication
- Light vaginal bleeding or discharge for a few weeks is normal
- Early movement is encouraged to prevent complications
Most women recover fully within 6 weeks. During recovery:
- Rest adequately
- Avoid heavy lifting and strenuous activity
- Resume sexual activity only after medical clearance
- Follow all post-operative instructions carefully
After recovery:
- Menstrual periods stop permanently
- Symptoms like pain or heavy bleeding usually resolve
- Pregnancy is no longer possible
- Menopause may occur earlier, depending on ovarian status
Many women experience significant improvement in quality of life. Emotional responses vary—some feel relief, while others may experience a sense of loss. Ongoing support and open communication with your doctor are essential.
