High Risk Pregnancy
What to Expect & How We Support You
High Risk Pregnancy
A high-risk pregnancy means that you or your baby may need extra care before, during, or after delivery. While the term can sound worrying, the right medical guidance, close monitoring, and timely intervention can significantly improve outcomes for both mother and baby.
Got Questions? We’ve Got Answers!
High-Risk Pregnancy & Advanced Maternity Care
A pregnancy is considered high risk when certain factors increase the chances of complications. These risks may be present before pregnancy or may develop during pregnancy. High-risk care focuses on early detection, prevention, and personalized treatment to ensure the best possible outcome.
Even in a high-risk pregnancy, there is a lot you can do to protect your health and your baby’s well-being:
Plan before pregnancy
A preconception consultation helps assess risks, optimize existing medical conditions, and start prenatal vitamins like folic acid.Attend regular prenatal check-ups
Frequent visits allow close monitoring of fetal growth and maternal health. You may also be co-managed with specialists if needed.Follow healthy lifestyle habits
Avoid smoking, alcohol, and unsafe medications. Always consult your doctor before taking any supplements or drugs.Manage existing medical conditions
Proper control of diabetes, blood pressure, thyroid issues, or other conditions is crucial during pregnancy.
Seek medical attention right away if you experience:
Vaginal bleeding or fluid leakage
Severe headaches or vision changes
Persistent abdominal pain or cramps
Reduced fetal movements
Burning or pain while urinating
Sudden swelling of face, hands, or fingers
Fever, chills, or repeated vomiting
Dizziness or emotional distress
Early reporting of symptoms can prevent serious complications.
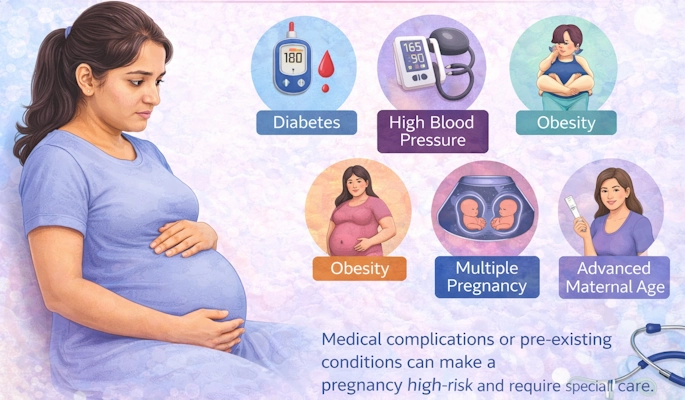
 You may be classified as high risk due to one or more of the following:
You may be classified as high risk due to one or more of the following:
Advanced maternal age – Pregnancy after the age of 35 may increase certain risks.
Lifestyle factors – Smoking, alcohol consumption, or drug use can affect fetal development.
Pre-existing medical conditions – High blood pressure, diabetes, obesity, thyroid disorders, heart disease, epilepsy, asthma, blood disorders, or infections.
Pregnancy-related complications – Placenta-related issues, restricted fetal growth, Rh incompatibility, or reduced amniotic fluid.
Multiple pregnancy – Carrying twins or higher-order multiples.
Previous pregnancy history – Prior preterm birth, preeclampsia, pregnancy-induced hypertension, or recurrent pregnancy losses.
Understanding your individual risk factors helps your gynaecologist create a tailored care plan for you.
Depending on your condition, your gynecologist may recommend advanced tests to closely monitor your pregnancy, such as:
Targeted or level-II ultrasound to assess fetal growth and development
Cell-free DNA (cfDNA) screening for chromosomal abnormalities
Amniocentesis or CVS for genetic testing when indicated
Cervical length ultrasound to assess the risk of preterm labor
Routine lab tests to screen for infections and urinary issues
Biophysical profile (BPP) and non-stress tests to monitor fetal well-being.
Your doctor will always explain the benefits and risks of each test, helping you make informed decisions with confidence.
What We Offer
Complete Women’s Healthcare Services
A full spectrum of gynaecologic and maternity services delivered with clinical precision and personalized attention.
Maternity Care
Comprehensive antenatal, delivery, and postnatal care focused on the health of both mother and baby.
Womanhood Care
Personalized gynaecologic care supporting hormonal, menstrual, and reproductive health at every life stage.
Invasive Surgeries
Advanced surgical procedures designed for precision, safety, and faster recovery.
Dedicated to Providing Quality Healthcare for All, Every Day
With the support of an experienced Dr. Sakshi Goel, many women with high-risk pregnancies go on to have safe and healthy deliveries.
